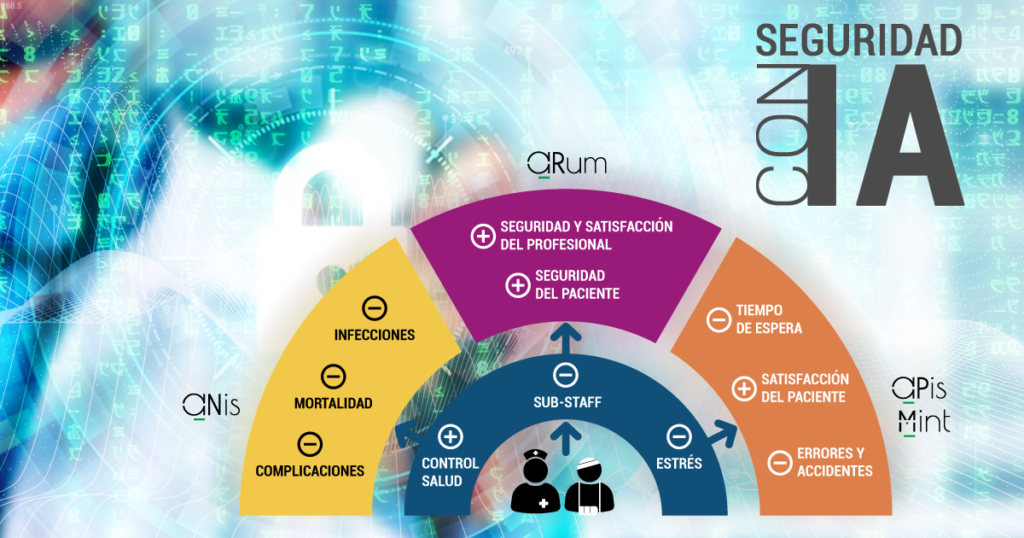
Patient safety is the reduction of the risk of unnecessary harm associated with healthcare to an acceptable minimum. It goes without saying that an essential factor in guaranteeing patient safety is that professionals also provide care in safe conditions.
Patient information makes it possible to detect problems, analyse pathologies, associations, comorbidities, therapeutic treatments, etc., but it also makes it possible to take preventive action. New technologies with Artificial Intelligence facilitate the identification of risks in order to develop more efficient preventive actions.
To increase safety, there are technological proposals such as new sensor devices, collection of a greater variety of data, software to generate alarms for unwanted events, and new products with Artificial Intelligence that allow the early detection of risks and are a support for the decision of professionals.
In this article we present the approach we are developing in Amalfi Analytics where we propose to use Artificial Intelligence to improve aspects of the management of patients, professionals and resources that, directly and indirectly, contribute to improve safety.
There are three unresolved management problems that have a huge impact on safety: excessive waiting times, sub-staffing and suboptimal management of chronicity.
We analyse each of these problems and explain how AI provides solutions.
Excessive waiting times in the different steps of the care process
Both in the emergency department and in the ward, excessive waiting times correlate, as has been shown in various publications, with more complications, hospital infections and mortality. Delays in transitions between care points (both from primary care to hospital and from hospital to socio-health care) also increase complications of all kinds. Finally, excessive waiting for surgery, both from the emergency department and waiting lists, often aggravates the patient’s condition.
AI provides predictive algorithms for emergency department activity (APIS) that aid planning and proactivity by reducing waiting times.
Amalfi’s solution anticipates the influx of patients by severity and type of patient, the occupancy of the different areas of the department, thus avoiding collapse, and the need for referrals to other centres and hospitalisation on the ward, managed with a Marketplace of resources (MINT). It warns of the expected pressure on the surgical block from the emergency department and the expected discharges from the different wards for the following day. In this way, the service manager can reorganise work, resources and staff, and coordinate with other hospital managers, sharing anticipated needs and problems.
With the use of this technology, we reduce waiting times in the emergency department by 25%, referral times between centres by 50%, and the bureaucracy associated with bed search by 80%.
Sub-staffing.
We use this anglicism to denote the under-staffing of the number or type of professionals who should be in a given place at a given time. This situation increases the risk of accidents and medical errors, in two ways: those that compromise the health of the patient (e.g., medication administration errors), and also those that affect the health of the professional (e.g., accidents at work). Sub-staffing also affects the mental well-being of professionals, who suffer from having to care for patients in poor conditions and from having to take on the work of two or three people. This leads to an increase in sick leave, unplanned absenteeism and burnout.
In this case, AI provides predictive absenteeism algorithms (ARUM) that are fed by the centre’s human resources data, and predict the number of unscheduled absences. These predictions are distributed by service, professional category and shift, with horizons ranging from 1 day to several weeks, with extraordinary accuracy (up to 97% at 1 week’s sight, on the number of absences). This makes it possible to anticipate coverage actions, avoid being left uncovered and manage shifts and work schedules more rationally in the short term. In the medium and long term, this technology makes it possible to anticipate the minimum number of temporary positions required over a horizon of several months, which makes it possible to improve the length of temporary contracts. All of this results in professional satisfaction and working conditions, as well as a reduction in recruitment costs.
Sub-optimal management of chronicity.
The difficulty of chronic process management includes its variability and multifactoriality, with social factors that are not easily taken into account in traditional clinical guidelines and protocols. This difficulty is addressed by stratification algorithms, which have often been designed for planning and health economics studies. But they are too granular to identify patient-specific risks and to help the practitioner formulate tailored treatment plans.
AI technology analyses data from a complex chronic process and discovers patterns or homogeneous clusters within it (ANIS). It refines stratification algorithms in that it identifies that each group found is characterised by distinct comorbidities and different risks. This allows for the creation of more refined or “semi-personalised” therapeutic guidelines, to treat “patients like this”. To do this, we use newly developed clustering algorithms that go beyond traditional statistical algorithms.
This new technology anticipates the temporal evolution of each patient pattern, in order to anticipate risks. This allows a territorial planner to draw up care plans appropriate to the needs of his population, favouring health monitoring and prevention.
The conclusion is that patient safety is one of the top priorities for Health Services that develop patient safety promotion and monitoring programmes. Health centres develop risk indicators and in addition to the direct actions of the safety programme, having AI tools will allow them to improve the outcome of the safety indicators.
It is necessary to promote the use of this new technology to increase both safety and patient and professional satisfaction, while reducing accidents and claims for the health centre.
AI allows healthcare systems to coordinate their different levels (hospital, emergency, nursing homes, primary care, etc.) and to take real responsibility for the entire patient journey. The system must react more specifically to a person’s real needs and condition on the basis of information from their medical records.
Finally, AI facilitates the rationalisation of the use of resources, which translates into savings, which in turn can be used to improve safety in other ways or to promote innovation in healthcare.
Bibliography
Publications that indicate how Machine Learning helps with the problems posed
[1] https://www.healthaffairs.org/doi/10.1377/hlthaff.2018.0738 , for patient safety
[2] https://www.nejm.org/doi/full/10.1056/NEJMsa0810119 , due to surgical complications
[3] https://journals.sagepub.com/doi/10.1177/000313481808400943 , more than surgical complications in the ER
[4] https://jamanetwork.com/journals/jama/fullarticle/188074 , due to medical errors
[5] https://www.nejm.org/doi/full/10.1056/NEJMsa0907115 , identification and medication errors
[6] https://www.nejm.org/doi/10.1056/NEJMoa1801550 , for infections
[7] https://onlinelibrary.wiley.com/doi/10.1111/acem.12876 , for infections in the ED
[8] https://www.researchgate.net/publication/270897505_Patient_Safety_An_unsystematic_review_and_bibliography , Emergency Review
[9] https://www.jointcommission.org/-/media/deprecated-unorganized/imported-assets/tjc/system-folders/topics-library/tjc-improvingpatientandworkersafety-monographpdf.pdf?db=web&hash=2772E4D4E100BCE47F47A47F47A47 for professional (and patient) safety
[10] https://academic.oup.com/occmed/article/67/1/52/2445871 , for absenteeism and burnout
[11] https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-020-05417-w , waiting time in the ER
[12] https://www.hcltech.com/blogs/ai-driven-digitization-chronic-disease-management-process , Automatic learning in chronicity
[13] https://www.redaccionmedica.com/secciones/enfermeria/cada-paciente-que-sobrecarga-a-enfermeria-aumenta-un-19-la-mortalidad-9152