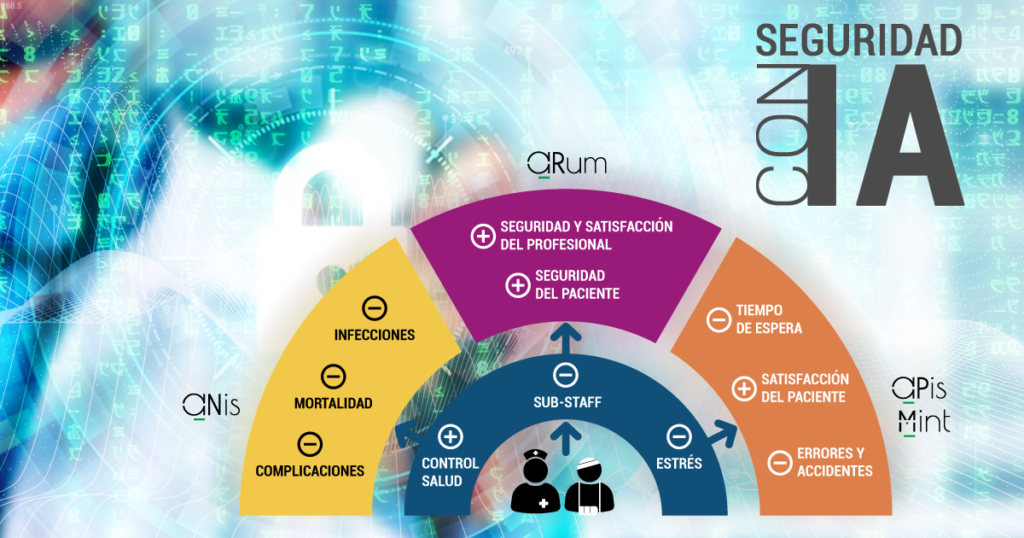
A reflection: IAR in health, only for clinical decisions?
Care management as the best entry point for Artificial Intelligence in hospitals. For years we have been witnessing progress in the application of Artificial Intelligence to precision medicine, but the first step must be precision management.
In a recent article in the prestigious Harvard Business Review, the authors make an excellent reflection on the digitisation of hospitals. From the same summary, their position is very clear:
“[In hospitals] the use of digital technologies for clinical decision-making has received the most attention. But they also have the potential to help make better decisions in many areas of operations.”
And they conclude by saying.
“Given the ageing population, the prevalence of chronic diseases and advances in medicine, it has become more important than ever for hospitals to operate efficiently and effectively. In the future, the key to improving operational decision-making will lie in their ability to join the digital transformation.”
The authors propose concrete tasks within hospitals that can be addressed with digital technologies:
- Estimating the number of arrivals, discharges and referrals from a service, to improve patient flows and reduce lengths of stay and waiting times.
- Prediction of absenteeism in nursing, in order to anticipate coverage and improve working conditions and recruitment.
- Generation of teams that optimally combine roles, skills and experience for a given task.
- Optimisation of timetables for the critical surgical area, which involves anticipating the duration of each intervention.
- Improvements in the medical and surgical supply chain, with technologies such as RFID, but also with improvements in the coordination of shipments and the prediction of demand and inventories.
Note that Artificial Intelligence (hereafter AI), and in particular Machine Learning (ML), is the central digital technology in all these applications.
In this note, we want to go further than the article cited above. Yes, the use of AI is possible and necessary also in hospital management problems. But we also argue that this is the easiest and fastest way to introduce AI in hospitals. Much more so than through diagnosis or patient-to-patient therapeutic recommendation, which are usually the flagship applications of AI in healthcare.
The most accessible AI for hospitals: applied to management problems
The main contribution of this column is to give in detail the reasons that lead us to this strong statement.
Ease of implementation. To develop these applications, only routine data are needed, such as the care activity data that are extracted for billing in the CMBD, or the human resources data that are already dumped in a structured manner in the hospital’s Datawarehouse. The IT department only has to schedule a regular retrieval of a query that they probably already have formulated for their day-to-day work.
In contrast, applications oriented to diagnosis or therapeutic recommendation of patients need to have all patient data, which are distributed among several non-interoperable silos. This makes any project expensive, time-consuming, and long-term.
Recycling routine data is much easier than integrating scattered data, let alone getting new data.
Scalability. By using existing and almost standardised data, applications can be deployed in large, medium and small hospitals and have an impact on the entire health system. The only requirement is the existence of a history of a few years, i.e. that the computerisation and registration are not too recent. Training Machine Learning models for these tasks requires a fairly moderate volume of data.
In contrast, patient-driven applications are usually only available to large, research-intensive and resource-intensive hospitals. We are talking about “Big Data” problems, as training Deep Learning models with images, natural language or omics requires large amounts of data. And it also requires the time of clinical specialists who, except in the largest centres, are not available for projects of this type.
Immediate results, better adoption. By addressing operational problems in the care process, users perceive an immediate improvement in their day-to-day lives, which favours adoption.
In contrast, when it comes to diagnosing or treating individuals, a system error can have lethal consequences. The clinician needs to have a great deal of confidence in the system, and to understand the reasons for the predictions it makes. Explainability and interpretability in ML is still a poorly established area, and models such as Deep Learning are notoriously opaque.
Fewer legal obstacles. As these are predictions of activity or about groups, the identity of the people involved (patients or professionals) is irrelevant. The data can be de-identified or even aggregated. It is only necessary, of course, to verify compliance with current legislation (GDPR) and the lawfulness of the processing by means of the corresponding risk and/or impact assessments.
In contrast, clinical decision support applications are usually considered medical devices and therefore need to be certified as such. This is a long and complex process. In many cases, the informed consent of the patients whose data will be used will be required, which is often costly or unfeasible.
Overall return to the institution. The results of improved management are beneficial for most patients and for most professionals. As implementation and adoption is easy, the ROI is high and close in time. Process improvement often frees up resources that can be used for continuous improvement and other innovation and continuous improvement projects.
In contrast, personalised diagnostic and treatment applications focus on niche patients or, at best, a single speciality. We are a long way from being able to design applications that diagnose well and recommend well for all patients. As these projects take months or years to implement, there is a high risk that they will be cancelled before they are finished, due to changes in priorities or lack of funding.
Conclusions
The famous goal of “putting the patient at the centre” can be achieved in several ways. With precision medicine, yes, but also by having well-established processes and by giving professionals the resources they need to do their job well. And these are management aspects.
Predictive machine learning for management problems helps to anticipate needs and create a good working environment for professionals. When people have the resources and are comfortable working, they are more productive, engaged in their work and even more creative and open to innovation.
The challenge, as with all technology, is to ensure that it is developed and implemented with the user in mind and as an imposition.
Going back to the Harvard Business Review article, we note that the authors point to these possibilities as ideas, or mention preliminary, almost research-like projects, applied in a single hospital. At Amalfi Analytics we have turned some of these ideas into reality. We have developed easy-to-use tools for a number of management problems, including predicting activity and needs in the emergency department and managing absenteeism in human resources. We have explained this in previous issues of this Hospitecnia newsletter [references 2-7].
References
[1] How Digital Transformation Can Improve Hospitals’ Operational Decisions, by Song-Hee Kim (Seoul National University) and Hummy Song (Wharton School, University of Pennsylvania), Harvard Business Review, Enero 2021, https://hbr.org/2022/01/how-digital-transformation-can-improve-hospitals-operational-decisions
[2] Urgencias hospitalarias más eficientes y seguras con inteligencia artificial. Laura Aviñó, Amalfi Analytics. Boletín Hospitecnia, Julio 2020.
[3] Aplicación de machine learning en la gestión de las personas con enfermedades crónicas. Francesc Güell y Martí Zamora. Boletín Hospitecnia, Septiembre 2020.
[4] Los profesionales, la clave del confort hospitalario. Jose Munuera, Amalfi Analytics. Boletín Hospitecnia, Octubre 2020.
[5] La sostenibilidad de la medicina a través del Machine Learning Marta Cornudella, Amalfi Analytics. Boletín Hospitecnia, Julio 2021.
[6] Hacia una gestión predictiva de urgencias: Desarrollo de una plataforma con Machine Learning en tiempo de COVID-19. Julianna Ribera y Ricard Gavaldà, Amalfi Analytics. Boletín Hospitecnia, Octubre 2021.
[7] Seguridad del paciente facilitada con IA. Ricard Gavaldà y Julianna Ribera, Amalfi Analytics. Boletín Hospitecnia, Enero 2022.